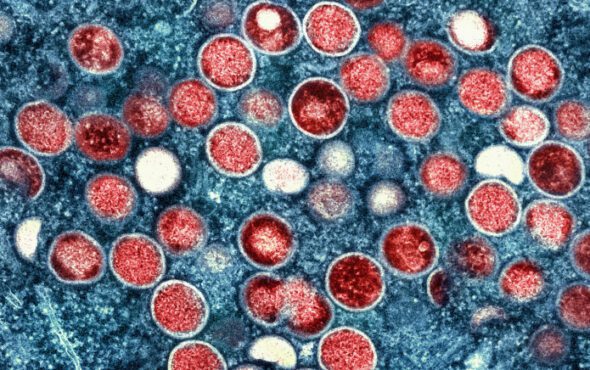
Concern is growing that the scramble for scarce supplies of monkeypox vaccines could see some nations and high-risk groups miss out – recalling unequal global access to COVID-19 vaccines and HIV medication.
The outbreak, which has reached nearly 100 countries outside of Africa, where the virus is endemic, is overwhelmingly being transmitted among men who have sex with men. They are getting priority for vaccination globally, but some face a longer wait than others.
“In a lot of ways we’re seeing history repeat itself, unfortunately,” said Wafaa El-Sadr, executive vice president for Columbia Global Centers, Columbia University’s international network of campuses.
“We have yet to learn the hard lessons we learned first from HIV and COVID-19 more recently,” she added.
Effective HIV treatments hit the market in 1996 and soon ended the crisis phase of the AIDS epidemic in Western nations, but it was years later before substantial antiretroviral supplies reached sub-Saharan Africa.
Similarly, COVID-19 vaccines and treatments were stockpiled by the richest countries.
Limited supplies of Bavarian Nordic’s monkeypox vaccine have mostly been snapped up by the United States – the country with the most cases, but some hard-hit nations such as Brazil and Peru still have none, the World Health Organization (WHO) has said.
The WHO is trying to set up an equitable distribution mechanism, but has no access to vaccines.
U.S. officials said on Aug. 26 that nearly 1.1 million vials of the vaccine – called Jynneos, Imvanex and Imvamune, depending on the country – have either been allocated to jurisdictions within the United States or are now available for ordering.
The country is home to more than 18,000 of the roughly 48,800 cases diagnosed in 99 nations during 2022, according to the U.S. Centers for Disease Control and Prevention (CDC).
This has left other nations to scramble for the remaining doses, even as scientists remain unsure how well the vaccine will work.
FAIR DISTRIBUTION?
Besides calling for fair distribution among newly hit countries, some experts say an equitable global response would also prioritise high-risk people in the 11 central and western countries in Africa where monkeypox has become endemic since first being identified in humans in 1970.
In Africa, however, some health officials see no urgent need to vaccinate against the virus, which spreads through very close contact, and has caused 15 deaths worldwide this year.
“Vaccine hoarding is always a concern … but for now, for Africa, the plan is not to distribute vaccines or vaccinate large numbers of people against a few cases of monkeypox which we have seen in the past,” Bartholomew Dicky Akanmor, adviser for vaccine research and regulation with the WHO’s Africa office, told the Thomson Reuters Foundation.
In Ghana, the director general of the country’s health service, Patrick Kuma-Aboagye, said that in contrast to COVID-19 “there is no cause for alarm”.
“We are monitoring and looking at the numbers and if we see a particular group at high risk, we will vaccinate as is being done in countries like the U.S.,” he added.
Within those countries that are vaccinating, experts are also warning about uneven access among certain groups – from those without an internet connection to undocumented migrants and people of colour.
In the United States, data indicates that, similar to HIV, monkeypox is disproportionately impacting Black and Latino men. Yet white men are more likely to access the vaccine.
In New York City, the epicentre of the U.S. outbreak with more than 3,000 cases here, recent data showed that while a respective 34% and 29% of monkeypox diagnoses have been among Latinos and Blacks, those groups have received only 23% and 12% of the available vaccine doses respectively.
“None of this should be surprising,” said David J. Johns, executive director of the National Black Justice Coalition in Washington, DC. “Healthcare in our country and responses to viruses are seldom democratised.”
New York City’s government has pledged $5 million to local community based organizations to promote vaccination among gay and bisexual men and transgender people of colour, as well as people of lower socioeconomic status.
The Biden administration has set aside 50,000 extra vaccine doses for localities that focus on providing vaccinations to members of the LGBTQ+ community here in a way that targets health inequities.
As a part of this pilot programme, it aims to provide on-site vaccinations at two major upcoming events that draw many LGBTQ+ of color – Southern Decadence in Louisiana, and Black Pride in Atlanta, said Deputy Coordinator of the White House monkeypox response, Demetre Daskalakis.
DIGITAL DIVIDE
Seeking to ensure limited supplies go where most needed in hard-hit western Europe here, the EU has bought 160,000 vaccine doses to share out among member states according to the number of registered cases.
In Britain, more than 30,000 people have received their first vaccine dose out of an initial batch of 50,000 doses, but supplies are set to run out before a new shipment of 100,000 doses arrives in September, the UK Health Security Agency said.
LGBTQ+ groups working with the British government to ensure the doses reach marginalised groups have voiced frustration, saying people without digital access are among those at risk of missing out.
“You need to be digitally engaged – and pushy almost – to get access, which we know from other aspects of healthcare and HIV prevention will disadvantage groups who face health inequality,” said Danny Beales, head of policy and campaigns at the Aids Trust charity.
Doses in Britain are primarily being administered through sexual health clinics and pop-up “super vaccination” events, which see a lower attendance by members of minority groups, said Will Nutland, co-founder of Prepster.
Instead, Nutland and a coalition of public health nonprofits have been organising smaller drop-in vaccination sessions aimed at men and trans people from ethnic minorities, including migrants, who might fear having their data registered.
Still, the biggest concern among most health advocates is simply the shortage of supplies.
“Services have run out and lots of them are closing walk-in access,” said Beales. “There simply isn’t enough vaccine to meet need and demand.”
Reporting by Benjamin Ryan and Lucy Middleton.
GAY TIMES and Openly/Thomson Reuters Foundation are working together to deliver leading LGBTQ+ news to a global audience.



